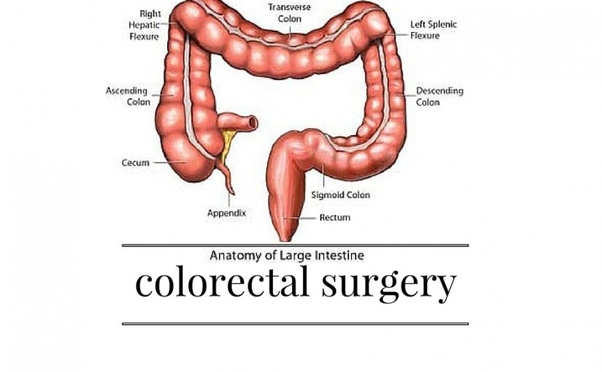
Colorectal Surgery

Causes of colorectal cancer
Colorectal cancer, also known as bowel cancer, colon cancer or rectal cancer, is any cancer (a growth, lump, tumor) of the colon and the rectum. The World Health Organization and CDC say it is the second most common cancer worldwide, after lung cancer.
A colorectal cancer may be benign or malignant. Benign means the tumor will not spread, while a malignant tumor consists of cells that can spread to other parts of the body and damage them.
Symptoms of colorectal cancer
- Going to the toilet more often.
- Diarrhea.
- Constipation.
- A feeling that the bowel does not empty properly after a bowel movement.
- Blood in feces (stools).
- Pains in the abdomen.
- Bloating in the abdomen.
- A feeling of fullness in the abdomen (maybe even after not eating for a while).
- Vomiting.
- Fatigue (tiredness).
- Inexplicable weight loss.
- A lump in the tummy or a lump in the back passage felt by your doctor.
- Unexplained iron deficiency in men, or in women after the menopause.
Causes of colorectal cancer
Experts say we are not completely sure why colorectal cancer develops in some people and not in others. However, several risk factors have been identified over the years - a risk factor is something which may increase a person's chances of developing a disease or condition.
The possible risk factors for colorectal factors are:
- Being elderly - the older you are the higher the risk is.
- A diet that is very high in animal protein.
- A diet that is very high in saturated fats.
- A diet that is very low in dietary fiber.
- A diet that is very high in calories.
- A diet that is very high in alcohol consumption.
- Women who have had breast, ovary and uterus cancers.
- A family history of colorectal cancer.
- Patients with ulcerative colitis.
- Being overweight/obese.
- Smoking. This study found that smoking is significantly associated with an increased risk for colorectal cancer and death.
- Being physically inactive.
- Presence of polyps in the colon/rectum. Untreated polyps may eventually become cancerous.
- Having Crohn's disease or Irritable Bowel Disease have a higher risk of developing colorectal cancer.